Attention Deficit/Hyperactive Disorder or ADHD is a serious public health problem that is affecting over 10% of children and millions of adults in the United States. Nearly half the children with ADHD grow up to be adults with ADHD.[2] This disease is characterized under mental disorders by the medical community, which attributes to its negative reputation among the general public. Children with ADHD can have difficulty performing well at schoolwork, making and keeping friends, and functioning in society.[1] Among Adults, ADHD may lead to anti-social behavior, substance abuse, anxiety disorder, stuttering and other speech and language problems.[3] After decades of study, the search for the cause of ADHD has come up to the new frontier of research, Epigenetics. But first, let us get to know what ADHD is…
ADHD often manifests as one of three types of behavioral disorders. These are:
| Disorder type | Symptoms in children |
| Attention Deficit type | Often doesn’t pay attention to details or makes careless mistakes in school work. |
| Often does not seem to listen when spoken to directly | |
| Often has trouble organizing activity. | |
| Often avoids, dislikes, or doesn’t want to do things that take a lot of mental effort or long period of time. | |
| Often easily distracted. | |
| Hyperactive/impulsive type | Often fidgets with hands or feet or squirms with sitting still is expected. |
| Often excessively runs about or climbs when and where it is not appropriate. | |
| Often has trouble doing leisure activities quietly. | |
| Is often “on the go” or acts as if “driven by a motor”. | |
| Often talks excessively, interrupts or intrudes on others. | |
| Combination type | Children with this type of disorder show significant degree of both attention deficit and hyperactive symptoms. |
Among adults, ADHD symptoms of childhood result in deficits in personal and social development. This is associated with fewer years of education, lower rates of professional employment, fewer social assets, and higher rates of separation and divorce.[4] Of the nearly 4.4% of adults who are affected with ADHD in the US, many live with coexisting mental and emotional disorders like depression and anxiety, as well as substance abuse disorders.[2]
For over five decades, scientists have been seeking the underlying cause of ADHD. It has been discovered that children with ADHD have structural and functional deficiency that can be correlated with behavioral problems. Children have smaller sized frontal lobe, right parietal cortex, caudate nucleus, cerebellum, and other regions of the brain5,6. These regions are involved in capacity to hold attention, learn new tasks, reasoning, problems solving, decision making and developing working memories. The overall smaller size of the brain is also associated with lower levels activity of neurotransmitters like dopamine and catecholamine in the brain. These stimulant neurotransmitters function as messengers between various parts of the brain. This deficiency represents widespread imbalance in the brain function. The stimulating functions of the brain regions that promote concentration, attention, learning, and memory are deficient; while, over-activity is present in regions of the brain associated with default, subconscious activity.[7] This leaves children unable to control impulses and focus.
In addition to widespread deficits, researchers have also discovered that ADHD can be inherited genetically. Children who have a parents or siblings with ADHD have a greater chance of developing ADHD compared to those without.[8] Thorough studies into genetics have found that there are many ADHD-related gene sequences that can affect dopamine, cathecholamine, and serotonin networks of the brain.[9] For a long time, genetics has been the dead end in the search for the cause of ADHD. Many have rejected the idea that we have capacity to influence changes genes and genetic information.
Though it is true that we cannot change genes, the emerging science of epigenetics is telling us that the environment can influence which genes are expressed. Researchers have discovered that everyone with genetic abnormality does not develop ADHD; rather, very few people with problematic genetic information express it.10,11 This leads to the question, why do some people express these genes, while most other don’t?
Epigenetics refers to the effect of the environment on physiological factors that control and influence genetic expression. The environment consists of everything that we are exposed to on a daily basis that is outside our bodies. Studies of epigenetics have revealed that children may be exposed to environmental factors that promote ADHD as early as during pregnancy, infancy, or during early part of childhood[12]. Here are some epigenetic factors that influence ADHD:
| Stage of Development | Environmental factors: |
| During Pregnancy and Newborn[12] | Exposure to substances like Nicotine, Alcohol, and recreational drugs. |
| Toxins like polychlorinated biphenyls (PCBs), hexachlorobenzene. | |
| Mother’s health related factors like stress, weight[13], diet[13], a
f glucocorticoids. |
|
| Early Childhood | Exposure to tobacco and lead[14] |
| Relational trauma causes maladaptive development of Infant nervous system.[15] | |
| Authoritarian parenting style16,17 |
All of the above environmental factors can be prevented. Factors like cigarette smoke, alcohol, and recreational drugs may be avoided, even with the help of medical intervention. Exposure to environmental toxin is a matter that must be addressed by public policy. On an individual level, exposure to toxins can be minimized through awareness, education, and seasonal detoxification practices.
While substances have their share of impact on the child’s brain development, the emotional experiences of the child are psychologically most important factors of brain development.[15] During pregnancy and the early years of the child’s life, the living environment is most often created by the parents. Parents also provide the emotional environment for the child’s development. Pregnancy is a period of the child’s development when the mother and the child share a blood supply. All the hormones and their cycles that occur in the mother’s body are also experienced by the child during the most vulnerable stage of its development. With due respect to this intimate relationship, Kaumāra-bhṛtya, the pediatric branch of Ayurveda, teaches profound ways to optimize the health of both parents, to support healthy conception and pregnancy, as well as post-birth care of the mother and child.
Researchers have also studied the relationship patterns between parents and child that promote ADHD. If the primary caregiver or parent of a child is unavailable or abusive towards the child, this has a negative impact on the parts of the brain related to social development of child. This has a negative impact on the child’s psyche; that leads to long lasting effects on the biochemistry of the immature brain.[15] Neglect or abuse from the caregiver are most powerful social or physical stressors for the developing brain.15 Outside of such extreme trauma, parenting styles can also place psychological stress on the child.
Children of parents with “authoritative parenting” style are more likely to have ADHD[16]. Authoritative parents often[18]:
- Have strict rules and expectations.
- Display little warmth and are highly controlling towards the child.
- Very demanding, but not responsive to the child’s needs.
- Use punishments with little or no explanation.
Such restrictive and aggressive behavior is outside of child coping capacity and causes significant psychological stress on the developing brain. Authoritative parenting style can also lead to other forms of emotional disorders like depression and anxiety.[16] A Korean study on parental attitudes revealed that affectionate parenting leads to better self-esteem in children with ADHD compared to controlling or rejecting parents. Parents with rejecting attitude were more likely to have children with lower social competence.[17] This study confirms the negative effects of aggressive, demeaning, or “hands off” parenting style on the mental health of the child. Therefore mindful and loving parenting is an essential part of the child’s healthy development.
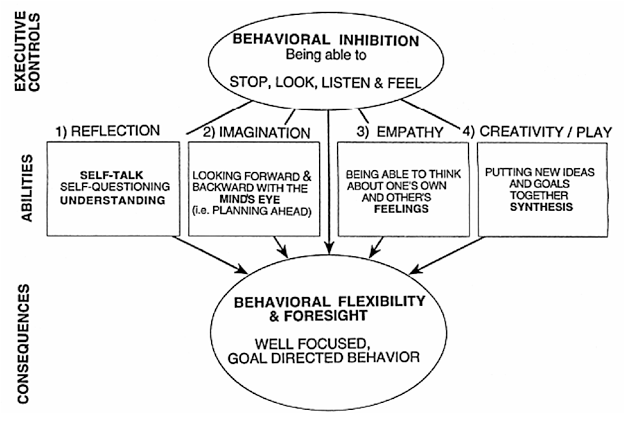
Optimizing parent-child interaction is an essential part of ADHD treatment. Clinically designed Behavioral parental training (BPT) programs have been shown to help reduce child’s tendency to have “hyperactive, defiant, and aggressive behavior”; BPT also improved parent behavior and reduced parent stress.[19] Such parental training has been shown to improve parental effectiveness, as well as children’s social skills and classroom behavior.[19] Play is also an important part of childhood development. It is proven essential for social maturation, attentional development, and emotional integrity. Playful interaction with parents, caregivers, friends, etc. is beneficial for healthy maturation of the mind. Play engages the frontal lobe of the brain and promotes development in the attentional and regulatory functions of the brain.[20] These functions of the brain allow us to “Stop, look, listen, and feel”. Figure below illustrates how these regulatory functions of “Stop, look, listen, and feel” translate into emotional development of the child.
Influence of the Methyltetrahydrofolate reductase (MTHFR) gene:
MTHFR is a critical enzyme for the methylation process in the body. Activity of this enzyme is required to make amino acid methionine, which is essential for normal activity of many proteins.[21] Methylation is also an important step in controlling gene expression. Abnormality in this gene has been associated with disorders like: Stroke, heart disease, high blood pressure, psychiatric disorders, and certain cancers.[21] In recent years, emerging evidence shows that ADHD may be affected by the activity of MTHFR. Children with lower methylation activity at birth have greater chance of developing ADHD symptoms by the age of 6.[22] Studies have shown specific mutations on the MTHFR gene have greater association with ADHD. 23,24
Low activity of MTHFR causes low levels of 5-Methyltetrahydrofolate (5-MTHF) in the body. Fortunately, 5-MTHF, which is product of MTHFR activity, can be easily supplemented.
Food and ADHD:
Food is an important source of nutritional medicine for the body. However, food allergies can put a lot of strain on the body. Allergies to foods and food additives are present in significant numbers among people with ADHD. In a study of children with ADHD, nearly 73% of children had allergies to foods, dyes, or other additives.[25] All children demonstrated improvement of symptoms with elimination of allergens foods or additives. Another study found up to 30% of cases of hyperactivity may be related with allergic reactions to artificial food colors.[26]
Sweet treats are often the favorite foods of many children. But, high refined sugar in diet can also lead to significant worsening of ADHD symptoms.[27] On the other hand; elimination of refined sugar from diet can lead to improvement of symptoms.[28]
In Summary:
Attention Deficit/Hyperactivity Disorder is a relatively common childhood mental health condition. It can affect the process of personal and social development of our precious children. However, there are some fundamental ways by which ADHD may be prevented. It is essential for the child to have a safe, healthy, and wholesome environment for normal growth. This calls on the parents, the families, and community to take responsibility for learning about and providing the best environment for the child’s growth. Some specific factors of this safe environment include:
- Healthy choices made by parents before conception, during pregnancy and after birth;
- Loving and emotionally available care-givers;
- Safe environment for play and happiness;
- Detoxification of the living environment;
- Periodic detoxification of the whole body.
Ayurveda teaches its patrons that, in order have a generation of healthy and whole-hearted children the whole society must participate in creating a healthy and whole-hearted environment. This requires collaborative action at parental, familial, community, and cultural levels. Coming together on all these levels is important to secure a bright future for our coming generations.
Herbal treatments for ADHD:
Ayurvedic herbs provide excellent options for managing various symptoms of ADHD. Ashwagandha, Brahmi, and Mucuna are essential nervine herbs that provide a multifaceted approach to treating an individual with ADHD.
Ashwagandha is an important anti-stress medicine, which has similar activity to GABA, a relaxing neurotransmitter for the brain.[29] Active compounds in Ashwagandha bind to GABA receptors in the brain, helping to curb anxiety and uplift mood, inducing relaxation. Traditionally, the herb is used to treat patient with mood disturbances.
Brahmi is tonifying herb that protects and nourishes the nerves, thus it supports normal nervous system activity. 90 day treatment with Brahmi has shown to improve working memory and accuracy of special memory in children with ADHD.[30] Another study demonstrated that a 5 and 12 week course of Brahmi also improved the function of Auditory Verbal Learning.[31] Brahmi also proved helpful in improving attentiveness among children with ADHD.32 When given in combination of Ginkgo, Bhrami also helped to improve planning and problem solving, information processing speed, motor responsiveness and decision making.[33] These improvements are indication of enhanced function of the brain due to the effect of Bhrami.
Mucuna is popular anti-parkinson due its high content of L-Dopa compound.[34] L-Dopa serves as precursor for dopamine, which is often depleted among children with ADHD. Improved dopamine levels in the brain help to promote better regulatory activity. Stimulant drugs like Ritalin and Vyvance, also exert their therapeutic effect by increasing dopamine availability in the brain.
Combined therapy with these herbs can very beneficial for both children and adults with ADHD.
Shirodhara: is the “method of pouring of cow milk or Tila tail over forehead of patients in the form of a regular stream from a specific height of about 3.14 inches as mentioned in classics in a fixed oscillatory movement for 45 minutes per day for two weeks.”[35] This therapy is well known for its relaxing effects as part of the post-Panchakarma treatment. Shirodhara treatments have proven to improve symptoms of ADHD, by reducing impulsiveness and hyperactivity in children.36, 37 Shirodhara therapy has a lasting nourishing and relaxing effect on the mind.
References
- [1] Center for Disease Control. Attention Deficit/Hyperactivity Disorder: Research Overview. CDC.gov, Feb. 20, 2014.
- [2] Kessler RC, et al.; The Prevalence and Correlates of Adult ADHD in the United States: Results from the National Comorbidity Survey Replication. American Journal of Psychiatry. 2006. 163: 724-732.
- [3] Biederman J, et al (1993): Patterns of psychiatric comorbidity, cognition, and psychosocial functioning in adults with attention deficit hyperactivity disorder. American Journal of Psychiatry 150: 1792–1798.
- [4] Faraone SV, et al.; Attention-Deficit/Hyperactivity Disorder in Adults: An Overview. Society of Biological Psychiatry, 2000; Vol. 48, Pg. 9-20.
- [5] Curatolo P, et al.; The Neurobiology of Attention Deficit/Hyperactivity Disorder. European Journal of Pediatric Neurology, 2009; Vol. 13, Pg. 299-304.
- [6] Krain AM and Castellanos FX. Brain development and ADHD. Clinical Psychology Review 26 (2006) 433–444
- [7] Aboitiz F, et al. Irrelevant stimulus processing in ADHD: catecholamine dynamics and attentional networks. Frontiers in Psychology, 2014; Vol. 5(183), Pg. 1-15.
- [8] Beiderman J. Attention-Deficit/Hyperactivity Disorder: A Selective Overview. Society of Biological Psychiatry, 2005; Vol. 15, Pg. 1215-1220.
- [9] Banachewski T, et al. Molecular genetics of attention-deficit/hyperactivity disorder: an overview. European Child and Adolescent Psychiatry, 2010; Vol. 19, Pg. 237–257.
- [10] Neale BM, et al.; Genomewide association scan of attention deficit hyperactivity disorder. American Journal of Medical Genetics, 2008; Vol. 147B, Pg. 1337–1344.
- [11] Sonuga-Barke EJS. Editorial: ‘It’s the environment stupid!’ On epigenetics, programming and plasticity in child mental health. Journal of Child Psychology and Psychiatry, 2010; Vol. 51(2), Pg. 113–115.
- [12] Mills J and Petronis A. Pre- and peri-natal environmental risks for attention-deficit hyperactivity disorder (ADHD): the potential role of epigenetic processes in mediating susceptibility. Journal of Child Psychology and Psychiatry, 2008; Vol. 49(10), Pg. 1020–1030.
- [13] Rodriguez A, et al.; Maternal adiposity prior to pregnancy is associated with ADHD symptoms in offspring: evidence from three prospective pregnancy cohorts. International Journal of Obesity, 2008; Vol. 32, Pg. 550–557.
- [14] Braun JM, et al. Exposures to Environmental Toxicants and Attention Deficit Hyperactivity Disorder in U.S. Children. Environmental Health Perspectives, 2006; Vol. 114, Pg. 1904–1909.
- [15] Schore AE. The Effects of Early Relational Trauma on Right Brain Development, Affect Regulation, and Infant Mental health. Infant Mental Health Journal, 2001; Vol. 22(1–2), 201–269.
- [16] Lange G, et al.; Family factors associated with attention deficit hyperactivity disorder and emotional disorders in children. Journal of Family Therapy (2005); Vol. 27, Pg 76–96
- [17] Oh Won-oak, et al.; Parenting of children with ADHD in South Korea: the role of socio-emotional development of children with ADHD. Journal of Clinical Nursing, 2012; Vol. 21, Pg. 1932–1942.
- [18] Kopko K. Parenting Styles and Adolescents. Cornell University Cooperative Extensions, 2007.
- [19] Modesto-Lowe V, et al. ADHD: Does Parenting Style Matter? Clinical Pediatrics, Nov. 2008; Vol. 47(9), Pg. 865-872.
- [20] Jaak Panksepp. Can PLAY Diminish ADHD and Facilitate the Construction of the Social Brain? Journal of Canadian Academy of Children and Adolescent Psychiatry, 2009; Vol. 16(2), Pg. 57-66.
- [21] Genetic Home Reference. MTHFR. National Institute of Health. Online article ;, July 2011.
- [22] van Mil NH, et al. DNA methylation profiles at birth and child ADHD symptoms. Journal of Psychiatric Research, February 2014; Volume 49, Pages 51–59.
- [23] Cem Gokcen, et al. Methylenetetrahydrofolate Reductase Gene Polymorphisms in Children with Attention Deficit Hyperactivity Disorder. International Journal of Medical Sciences, 2011; Vol. 8(7), Pg. 523-528.
- [24] Spellicy CJ, et al. Folate Metabolism Gene 5,10-Methylenetetrahydrofolate Reductase (MTHFR) Is Associated with ADHD in Myelomeningocele Patients. PLoS ONE, January 2012.
- [25] Boris M and Mandel FS. Foods and additives are common causes of attention deficit hyperactivity disorder. Annals of Allergy, Oct. 1994; Vol. 73, Pg. 462-467.
- [26] Schab DW, Trihn NT. Do artificial food colors promote hyperactivity in children with hyperactivity syndromes? A metaanalysis of double-blind placebo-controlled trials. Dev Behav Pediatr 2004; Vol. 25, pg. 423–434.
- [27] Schnoll R, Burshteyn D, Cea-Aravena J. Nutrition in the treatment of attention-deficit disorder: A neglected but important aspect. Appl Psychophysiol Biofeedback 2003; Vol. 28, Pg. 63–75.
- [28] Rojas NJ, Chan E. Old and new controversies in the alternative treatment of attention deficit hyperactivity disorder. Mental Retard Develop Disabil Res Rev, 2005; Vol. 11, Pg. 116–130.
- [29] A.K. Mehta, et al.; Pharmacological effects of Withania somnifera root extract on GABA receptor complex. Indian J Med Res., Aug. 1991; Vol. 94, Pg. 312–315.
- [30] Stough C, T et al. (2001) The chronic effects of an extract of Bacopa monniera (Brahmi) on cognitive function in healthy human subjects. Psychopharmacology (Berl). 156(4):481-84.
- [31] Negi KS, Singh YD, Kushwaha KP (2000) Clinical evaluation of memory enhancing properties of Memory Plus in children with attention deficit hyperactivity disorder. Ind J Psychiatry 42(2) supplement. 6.
- [32] Con Stough et al (2008) examining the nootropic effects of a special extract of Bacopa monniera Linn. on human cognitive functioning: 90 day double-blind placebo-controlled randomized trial. Phytother Research 22(12):1629-34.
- [33] Nathan PJ, et al. Effects of a combined extract of Ginkgo biloba and Bacopa monniera on cognitive function in healthy humans. Human Psychopharmacology: Clinical and Experimental, 2004; Vol. 19(2), pages 91–96.
- [34] Manyam BV, et al. Effect of antiparkinson drug HP-200 (Mucuna pruriens) on the central monoaminergic neurotransmitters. Phytotherapy Research, Sept. 2004; Vol. 18(9), pages 706–712.
- [35] Kumar SH, et al. Recent researches on Ayuvedic management of Attetion Deficit Hyperactivity Disorder (ADHD) in children – A Review. PunarnaV Ayurved Journal, Dec. 2013, Vol. 1(1), Pg. 55-64.
- [36] Singhal HK, Neetu, Kumar A, Rai M (2010) Ayurvedic approach for improving reaction time of attention deficit hyperactivity disorder affected children. AYU 31 (3) 338-42.
- [37] Ojha N and Kumar A (2007) Clinical study on the role of an ayurvedic compound (Manas Niyamak Yoga) and shirodhara in the management of ADHD in children; Journal of Ayurveda 1(1)39-47.

Recent Comments